Opioid addiction in Canada has many faces. It is Benjamin, who was prescribed opioids for dental pain and then discovered that they helped him cope with the memories of childhood trauma. It is Greg, who woke up one morning and found his wife dead from an accidental fentanyl overdose. It is Sean, who turned to alcohol and opiates when he lost his pregnant girlfriend in a drowning accident.
The tragedy of opioid addiction is woven through the stories of those who are addicted, the loved ones who are supporting them, and the doctors and social workers who are trying to help them. Some of these stories – including those mentioned above – have been compiled in The Opioid Chapters, a project that attempts to shed light on the humanity of a crisis that is often reduced to statistics.
A Double-Edged Crisis
Addiction to prescription opioids is not as simple to analyze as addictions to other substances. It is easy for us to say that street drugs like heroin and cocaine destroy lives. And this is true: there is no circumstance in which using these drugs contributes to a person’s overall state of health and wellness.
The same cannot be said of prescription opioids, because when used in accordance with medical guidelines, these can provide significant quality of life to people who would otherwise have none. What this means is that society has to strike a balance between solving the opioid addiction crisis and ensuring that the people who need to use the drug for legitimate medical purposes have access to it.
When Does Medicine Become A Drug?
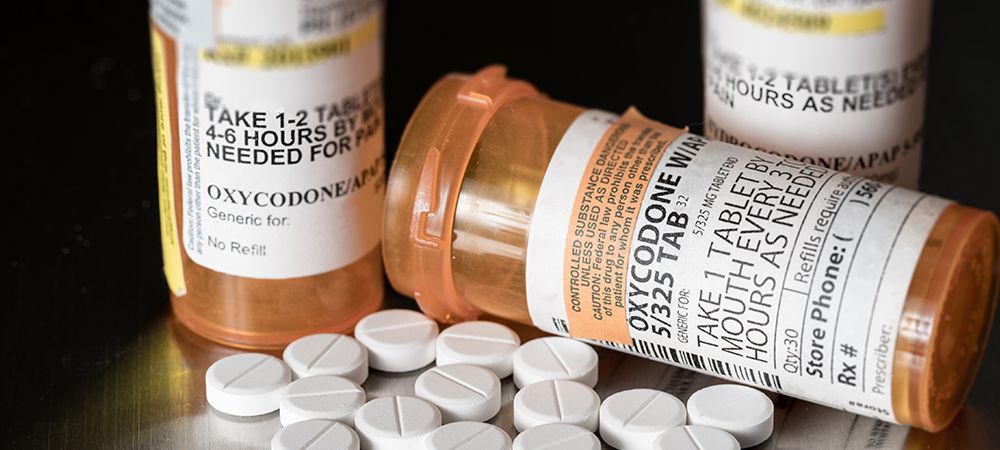
The term “opioids” is generally used to refer to prescription medication that is used to block pain signals between the brain and the body. Opioids that are commonly prescribed include oxycodone, morphine and fentanyl. They are typically used for short term management of chronic pain, pain relief following surgery, and management of pain resulting from cancer.
The risk of addiction arises from the fact that as the medication blocks pain signals, it boosts feelings of pleasure. In an individual who is struggling with trauma memories or stress, this can be dangerous: what starts off as a pain relief medication becomes a substance that is used to help the person function mentally or emotionally.
As the individual uses the opioid medication for a longer time, they may start to increase the dosage to achieve the same effects. And as the doses and frequency of use increase, so does the risk of decreased heart rate and breathing. This can lead to death. Add other substances like alcohol into the mix, and the danger increases exponentially.
The True Cost Of Opioid Addiction
According to the Canadian Centre on Substance Use & Addiction (CCSA), there were over 15,000 opioid-related deaths in Canada in the years 2016-2019. Over the last five years, emergency room admissions resulting from opioid harm have increased by 27%. It is estimated that in Ontario, the number of opioid-dependent people who gave birth to babies was 16 times higher in 2014 than in 2002. Many of these babies had to be treated for neonatal withdrawal.
The human cost of opioid addiction is undeniable. In addition to the lives lost, there are the lives permanently altered by disability or illness, loss of a loved one, and the breakdown of relationships.
The Centre for Addiction & Mental Health (CAMH) estimates that mental illness and addiction costs the Canadian economy more than $50 billion per year. This includes lost productivity and the costs of healthcare and social services. With an annual amount of $3.5 billion, opioids contribute to the third biggest substance-related cost in Canada, behind alcohol and tobacco.
First, Do No Harm
The obvious answer to this crisis would seem to be, “Let’s get people the help they need.” While society should always have a goal of helping people who are vulnerable, this is not quite as simple as it sounds.
One of the problems is stigma. Although we have come a long way in terms of societal attitudes to addiction, we have not quite managed to let go of the idea that equates addiction with irresponsibility. We routinely see people with addictions being referred to as “junkies” or “deadbeats”, instead of being treated as human beings worthy of being helped.
The tragic reality is that many people who want to seek treatment for addictions hesitate for fear of being ridiculed or rejected. In a lot of cases, trauma has brought them to the point of addiction: having been hurt by some element of humanity, they do not have faith that humanity will treat them with empathy.
Another problem is access to services. Not everyone has the financial means to go to rehab. Not everyone has the option of stepping out of their lives to go into a treatment centre, and when they do, they may find that treatment centres are full.
Therefore, while it is important to ensure that as much help as possible is available for people with opioid addictions, this does not go far enough. We also need to use harm reduction strategies to protect people who use opioids from serious harm or death. Some of these strategies can also serve as a first step in a drug rehab process.
Naloxone
Freely available in most parts of Canada, naloxone is a short-acting opioid antagonist that binds to the opioid receptors, thereby preventing other opioids from binding. This can rapidly reverse the potentially fatal effects of opioid overdose, such as depressed breathing and heart rate. When given soon after possible overdose events, naloxone can save lives. It should be noted that even when naloxone is administered, the individual should receive emergency care as soon as possible, since the effects of naloxone are not long-lasting.
Medication-Assisted Treatment
Unsupervised opioid withdrawal can be dangerous and uncomfortable. Individuals who want to break the hold of opioids on their lives may benefit from medication-assisted treatment, in which they are given longer-acting opioids that have less intense euphoric effects. This allows the person to start rebuilding their life while avoiding the worst of the withdrawal symptoms.

Public Education
One of the most powerful harm reduction strategies for any addiction is educating members of the community about the signs and symptoms of overdose, what to do in the event of such an emergency, and what sequence of events is set in motion when someone calls for help. A lot of people are hesitant to help those who are experiencing overdoses because they fear arrest by the police or stigmatization from family members. Humans have demonstrated over and over again that we fear what we do not understand: public education can reduce the anxiety about assisting people who need it.
Approaching Opioid Addiction Rehab With Empathy
The key to helping people with opioid addictions is empathy. Whether the situation calls for immediate harm reduction or longer term rehab, it is important for the individual to feel that they are in a safe place that is free from judgment, where they will receive the treatment they need.
If you decide that inpatient addiction rehab is the right choice for yourself or a loved one, 1000 Islands Rehab Centre will provide a healing environment, compassionate addiction treatment professionals, and a rehab program that is tailored to your unique needs and circumstances.
It is never too soon or too late to get help. Reach out to us today to begin your journey to recovery.
Related article: What is Medication-Assisted Treatment for Opioid Addiction? | 1000 Islands Addiction Rehab Centre (addictions.ca)